A New Standard in Patient Care
Our simulations increase team performance, address communication dynamics, reduce medical errors, and prepare your staff using life like rehearsals for the high-consequence, low-frequency emergencies that cost lives. The new way to train is here.
The Science of Medical Simulation
At Best Practice Medicine we take the science and research of simulation very seriously. Evidence-based medicine is at the heart of all that we do. Using cutting edge technology and teaching pedagogy, we stay up-to-date with the best practice in patient care and in teaching.
Reduce Preventable Medical Errors
Simulation-based training has been institutionalized in other high-hazard professions, such as aviation, nuclear power, and the military, to maximize training safety and minimize risk. Health care has lagged behind in simulation applications for a number of reasons, including cost, lack of rigorous proof of effect, and resistance to change.
What is High-Fidelity Simulation?
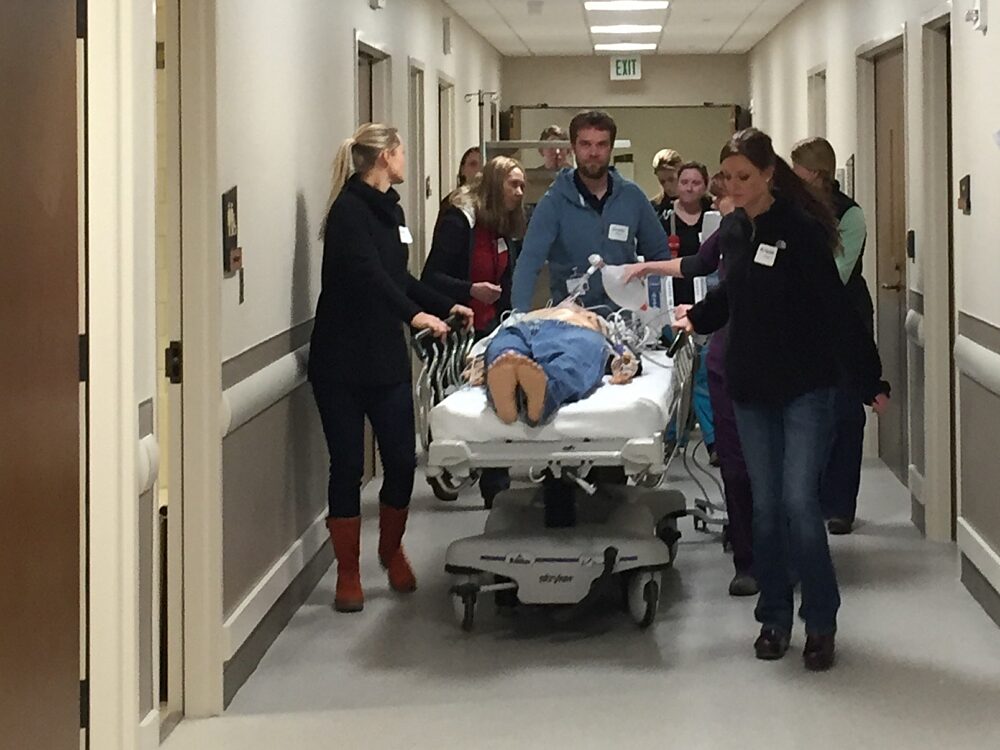
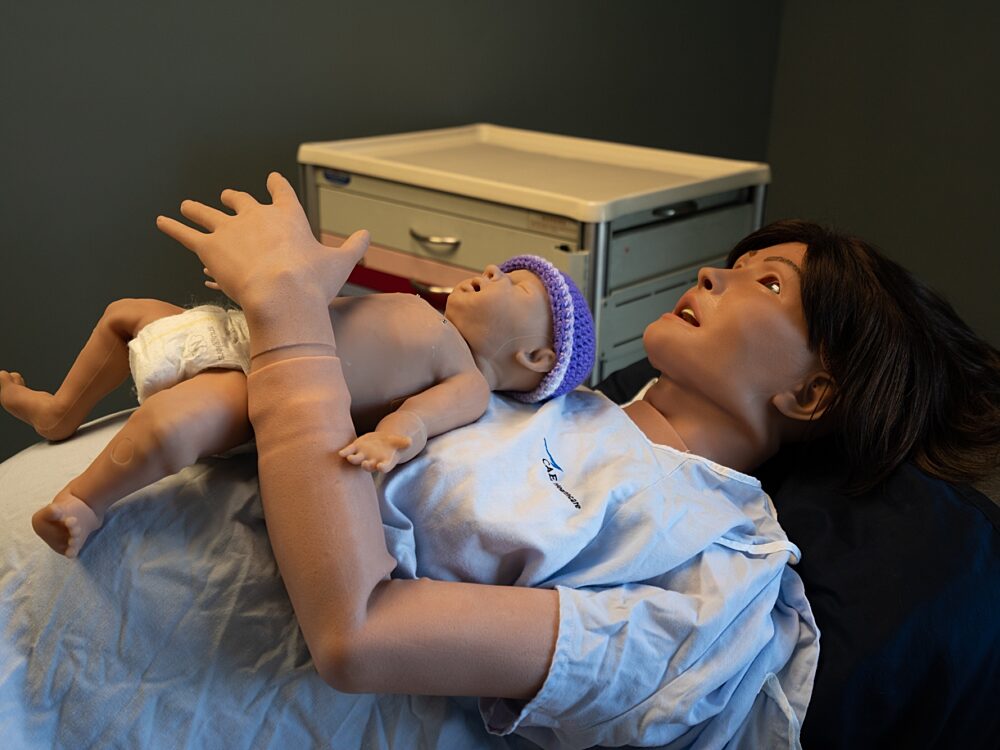
Most of us remember taking a CPR course when we practiced on "Dead Fred," a lifeless, limbless torso of foam. This teaching practice is in a sense medical simulation. However, the realism of this patient, and therefore the reality of the scene, is impaired by the fact that our patients are not in fact limbless plastic torsos. By integrating state-of-the-art simulator mannequin technology and employing an elite team of certified simulation specialists, we break this barrier and we train providers with a higher caliber of realism. These simulator mannequins take the place of real patients, so when providers make a mistake they can learn from it without risking the life of a father, daughter, neighbor, or friend. With life-like anatomical structures, actual pulse points, reactive and adaptive responses to treatment, and so much more, we can control the scene 100% and truly focus on objectives and experiential learning.
Simulation-based training has been institutionalized in other high-hazard professions, such as aviation, nuclear power, and the military, to maximize training safety and minimize risk. Healthcare has lagged behind in simulation applications for a number of reasons, including cost, lack of rigorous proof of effect, and resistance to change. Effective training has been shown to improve care and outcome, decrease litigation claims, and reduce sick leave. To be effective, training should be incentivized, in a realistic context, and delivered to inter-professional teams similar to those delivering actual care. Teamwork training is a useful addition, but it should be based on the characteristics of effective teamwork as derived from the study of frontline teams. Implementation of simulation and teamwork training is challenging with constraints on staff time, facilities, and finances. Local adoption and adaptation of effective programs can help keep costs down and make them locally relevant while maintaining effectiveness.
Why High-Fidelity Medical Simulation?
Short answer? Because it works. Recent studies show alarming rates of medical error in even the most developed healthcare systems. Preventable medical errors account for more than 400,000 deaths every year in the US alone (1). Best Practice Medicine was founded out of this understanding: there are good providers in this world harming patients because of bad decisions made out of a lack of meaningful continuing education. Simulation has been proven to reduce these medical errors and better prepare providers for those high-consequence patient encounters that only happen once in a blue moon. Now, you don't have to take our word for it. We may be pioneering the was simulation is delivered to rural and frontier settings, but there is an extensive body of knowledge which has closely studied the positive effects of simulation for years. At the end of the day, we believe, we know that providers care about doing their best, so take your care to the next level by practicing the way you practice.
Simulation Is Demonstrated To:
Reduce Preventable Medical Errors
Simulation-based learning can help mitigate this tension by developing health professionals' knowledge, skills, and attitudes while protecting patients from unnecessary risk. Simulation-based training has been institutionalized in other high-hazard professions, such as aviation, nuclear power, and the military, to maximize training safety and minimize risk. Health care has lagged behind in simulation applications for a number of reasons, including cost, lack of rigorous proof of effect, and resistance to change. Four themes provide a framework for an ethical analysis of simulation-based medical education: best standards of care and training, error management and patient safety, patient autonomy, and social justice and resource allocation. The use of simulation wherever feasible conveys a critical educational and ethical message to all: patients are to be protected whenever possible and they are not commodities to be used as conveniences of training. (1)
Improve Patient
Outcomes
Effective training has been shown to improve care and outcome, decrease litigation claims and reduce sick leave. To be effective, training should be incentivised, in a realistic context, and delivered to inter-professional teams similar to those delivering actual care. Teamwork training is a useful addition, but it should be based on the characteristics of effective teamwork as derived from the study of frontline teams. Implementation of simulation and teamwork training is challenging, with constraints on staff time, facilities and finances. Local adoption and adaptation of effective programs can help keep costs down, and make them locally relevant whilst maintaining effectiveness. Training programs need to evolve continually in line with new evidence. To do this, it is vital to monitor outcomes and robustly evaluate programs for their impact on patient care and outcome, not just on participants. (1)
Prepare Teams For High Consequence Care
Leaders in medical education have proposed that simulation-based assessments are essential to solving some of these challenges, given that they permit the testing of learners’ performance in safe and standardized environments. However, before an assessment tool is widely implemented, the validity evidence supporting both its intended use and the interpretation of its scores needs to be established. A recent systematic review of 417 studies of simulation-based assessments highlights notable limitations in the validity evidence supporting such tools. Simulation-based assessments often correlate positively with patient-related outcomes. Although these surrogates are imperfect, tools with established validity evidence may replace workplace-based assessments for evaluating select procedural skills. (1)
Testimonials
Our Process
It's what sets us apart
World Class Service
From the first moment you call Best Practice Medicine you can expect the highest quality of service possible. Our team utilizes multi-faceted communication and sophisticated client tracking software to provide timely communication with all clients of any size.
Dedicated account managers work directly with clients to identify needs, negotiate contracting, and advise on services. Your account manager is with you every step of the way so we can adapt services as needed.
24/7 support through our Emergency Operations Command (EOC) provides customer support any time of day or night.
Comprehensive Needs Assessment
With the understanding that every industrial environment is unique, we know a cookie-cutter solution won't meet your needs 100%. With that in mind, we approach every new client or project with a non-biased and flexible perspective.
A virtual or onsite needs assessment brings to light areas where your organization can be best supported by BPM. These findings help define the services needed by each individual client so when contracting begins, you know the solution is built for you.
Once an account manager is assigned to your organization they will reach out to discuss and confirm the services we can provide.
Contracting Transparency
Hidden fees, sleazy salesmen, and dishonest pricing have no place at Best Practice Medicine. As a small start-up business, we know how troublesome these suspect business practice can be.
We believe in contract transparency, so our clients know exactly what each penny they are paying is going towards. Varying contract and pricing models can be used to suit your needs best. BPM is a strong proponent of Cost-Plus pricing because it is simple and straightforward, and it focuses on your particular needs rather than the industry as a whole.
Our bottom line isn't the pennies in our bank account, but the patients who return home to their families.
Simulation In Action:
Research on Simulation
As an official Provisionally Accredited Simulation Program, we at Best Practice Medicine take the Science & Research of Simulation very seriously. Here you will find a host of clinical resources and white papers on the vital subject and efficacy of simulation in healthcare. These resources, updated regularly, are for your information and education—to help you better understand the science behind medical simulation and to accredit your knowledge if you are looking to add simulation to your organization's regular training and education.
For additional questions or inquiries into how we can help bring high-fidelity simulation to your team or organization, please don't hesitate to contact us.